Told by her partner, Sharon
“Shirley May Lamb was my same-gender life partner. She was a kind, intelligent, and resourceful woman who loved life and was active in a range of activities: gardening, baking, swimming, camping, etc. She did these things and more while living with Chronic Obstructive Pulmonary Disease (COPD) and being legally blind due to macular degeneration. She was described as “a young 81” and was an activist for women, LGBTQ+, the disabled community, and seniors. I was 69 at the time of her death. I’m a doctorally-prepared nurse and I was Shirley’s chosen decision-maker via a Section 9 Enhanced Representation Agreement (E-RA), conferring me with the power to make decisions on her behalf for routine care and also resuscitation, advanced care, and life support.
People with COPD experience exacerbations involving respiratory difficulties. There is a home care management program that was recommended for Shirley by a pulmonary specialist, but her family doctor refused to consent to it. I would only after her death discover that he believed she had an adenocarcinoma (a lung cancer), a diagnosis hidden from us, thereby preventing us from choosing treatment options. We turned to the doctors and staff in the Cowichan District Hospital’s (CDH) Emergency Department as our trusted alternative to the family doctor we had tried, unsuccessfully, to replace.
In May 2015, Shirley was admitted to CDH with suspected pneumonia. Her family doctor accused her of being “too costly” and “a drain on health care resources”, citing the use of the ER. Shirley was not dying. She was talking and trying to joke a bit out of nervousness. I insisted upon full care with a trial on a ventilator, in the event of a crisis, and was told by the family doctor that this made Shirley a DNR-3. That was not true. There were forms for this and he withheld them, signing my name rather than showing me the descriptions of intervention levels. I requested information about her care such as her medications, tests, treatments, and plans, and he refused, saying, “I will tell you what you need to know!” I saw deterioration in Shirley consistent with her receiving drugs that she did not tolerate. I saw and reported that she was not getting her critical medications. When I confronted the nurse, she threw Shirley’s nebulizers on the floor and remarked, “Now she will wait until the next dose”, which wouldn’t be until 8 hours later.
The woman visiting her mother in the bed across from Shirley then remarked, “You have to watch your step; otherwise, they will punish her again by withholding medications.” She added, “If you try to take her out, security will take you down.”
Shirley was struggling to breathe. She was deprived of fluids and her essential medications. I carried an oximeter and found her oxygen saturations to be out-of-range and potentially lethal for her.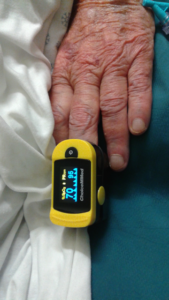
Shirley had been subjected to stealth euthanasia, a deceptive practice in hospitals whereby those with cardiac and chronic lung conditions are euthanized by juggling oxygen saturations outside of safe ranges, withholding essential drugs, administering drugs such as opioids, and withholding fluids to cause dehydration. It’s a practice applied to rid hospitals of patients deemed as “bed blockers”—the disabled, the elderly, and the chronically ill.
In September 2015, Shirley suddenly had severe back pain at home, rendering her unable to rise from bed. She was brought to the ER and admitted to the second floor again. The same problems began again with a new doctor, a locum for the previous family doctor, who ordered drugs that had Shirley delirious, struggling in bed, tossing side to side, and trying to rise while struggling to breathe. She had been given morphine, dexamethasone, and an insufficient dose of her nebulizers and I insisted on stopping the drugs causing the distress. Shirley recovered and was ambulatory and fit for discharge; then the original family doctor returned, designating her as “irreversible”. He again berated her for being “too costly” and said she had “no quality of life” because she was “disabled”. He did not do a single assessment of her again and was delaying her discharge unnecessarily. Shirley had proven on passes—home to work in the garden, out to Tim Horton’s—that she was fine for discharge. She was at risk of hospital-acquired infections (HAIs). She contracted a urinary tract infection (UTI) from being catheterized unnecessarily and left untreated. I took Shirley to the door to leave, again accusing the doctor of neglecting Shirley and insisting on her discharge in order to get her to another doctor. He blocked us! He wrote in the chart that he negated the Enhanced Representation Agreement, which he did not legally have the power to do, and yet it was done. Shirley was begging to go home. I was called away to speak with another MD whom I hoped might help us. But no help ever came.
In my absence, Shirley was given drugs rendering her unresponsive. Drugs that are used in Medical Assistance in Dying (MAiD) and for euthanizing patients. This was 2015 and MAiD was not yet legal. My partner did not die a natural death. She was killed by her physician who “doctored” the medical records, claiming care he never provided. The medical records revealed that he had been monitoring and charting a lab result for days, a result signifying that action should have been taken for a cardiovascular problem. He noted he was watching it and he intentionally did nothing. That inaction resulted in hours of pulmonary distress with calls to him from nurses, and he never came to see Shirley. He faxed in orders for Lasix without conducting tests, treatments, and assessment while she was in respiratory distress. This is while she was simultaneously given morphine, which is a drug that should not have been administered while in respiratory distress.
I have a file with the RCMP for a criminal investigation of her death, but all the investigations in the world will not bring her back to life. She died the victim of intersectional discrimination and a doctor toadying to administration, sacrificing Shirley’s life for cost containment. Unconscionable!
No one would help Shirley. In the hospital, I appealed to other doctors to tell me if there was something in the chart because the family doctor only said, “It’s something else,” when refusing Shirley care in an emergency. The ER doctor shook his head and said, “I can only tell you what I see and she has pulmonary edema.” I appealed to the unit manager, the community manager, the palliative doctor, as well as other doctors in the practice, and they all referred me back to the same family doctor. For people to threaten to arrest me for seeking help in an emergency, they had to be aware that this was deliberate, and they let it happen. It is a clear example of a culture of silence and self-protection.
Two submissions to the Patient Care Quality Office were useless courses of action. The Cowichan District Hospital spokespersons denied some claims and chose to ignore others, such as the order for the terminal sedation. The second submission was a detail of infractions of the responsibilities of nurses and specifics to be reported to the College of Registered Nurses of BC (CRNBC). That was also ignored. The CRNBC told me, “They can’t withhold the nurse’s name; we can get it from the chart” Well, it’s illegible and to this day, I still do not know the nurse’s full name who deliberately threw Shirley’s medication on the floor.
The RCMP told me they’re “busy” and just to speak to Victim Services. My partner’s life was treated as if she were a piece of rotting fruit to simply be tossed aside.
I pursued all the available investigative channels and it was completely dismissive and insufficient. While in CDH, I appealed to Shirley’s lawyer to help us. He advised me to tell them that I’m the Medical Rep, so that the situation may be navigated more smoothly. He asked for the MD’s name and when I gave it to him, he threw up his arms and exclaimed, “I am VERY familiar with him!” He further went on to say that he thought the doctor was “warehousing the elderly to die”. Unfortunately, he declined to help me, saying, “It’s a small town and I could lose business.” Every lawyer I wrote to and spoke with either referred me to the BC College of Physicians & Surgeons or told me they don’t deal with medical/physician suits.
One legal firm and a lawyer in Victoria said it sounded like a criminal case and to get a case number from the RCMP to investigate it. The constable suggested it might be criminal negligence, and I suggested there was evidence confirming malice aforethought, intent, advance planning, and motives of discrimination and cost-containment, which can all add up to a culpable homicide, specifically murder in the first degree. The law librarians were great. Never in fifty years of nursing have I ever seen such condoned harm-doing and such a system of legal impotence when the perpetrator is privileged and in a position of power and trust. The law, on paper, is clear: when a homicide is committed by a person in a position of trust, the punishment should be the maximum sentencing. I’m not giving up.
I first heard of The BC Wrongful Death Law Reform Society by watching the BC Legislature and seeing the organization introduced there. I wrote and was pleasantly surprised to find that the society members were interested in helping us and were well-informed about a range of problems from wrongful deaths involving accidents on the road to deaths from inadequate health care. They are professional, dedicated, informative, and have a comprehension of wrongful deaths from personal experiences. I am so thankful to have connected with this Society.
Where the root cause of lack of accountability comes from is the fact that anyone who does not meet the discriminatory criteria of having an income plus dependents has no “worth” under BC’s wrongful death laws. Shirley was a senior who was disabled and because she was “free” to be killed under the law, there was no civil legal deterrence mechanism in place to prevent this malicious doctor from behaving so recklessly so as to ensure my partner Shirley was deliberately killed. Only when all lives in BC have “worth” under the law, will incidents like this be deterred from happening through civil legal consequence. I feel that the Patient Care Quality Office and the RCMP were dismissive and woefully inadequate with respect to obtaining justice for Shirley. I’ve also been robbed of a democratic right to justice and accountability through civil means that would have otherwise been afforded to me in other jurisdictions.
BC is a beautiful province, and I hope we can change our wrongful death laws so as to avoid such reckless discrimination and lack of accountability in the future.”





 ‘In Their Name’ is the campaign of ‘The BC Wrongful Death Law Reform Society’ – a BC registered non-profit organization comprised of volunteer families who have lost a loved one to wrongful death in BC and were denied access to justice. In response to the biggest human rights issue facing the province today, our goal is to modernize British Columbia’s antiquated wrongful death legislation, which predates confederation (1846). Under current legislation, the value of a human life is measured only by the deceased’s future lost income, so long as they had dependents.
‘In Their Name’ is the campaign of ‘The BC Wrongful Death Law Reform Society’ – a BC registered non-profit organization comprised of volunteer families who have lost a loved one to wrongful death in BC and were denied access to justice. In response to the biggest human rights issue facing the province today, our goal is to modernize British Columbia’s antiquated wrongful death legislation, which predates confederation (1846). Under current legislation, the value of a human life is measured only by the deceased’s future lost income, so long as they had dependents.